Facial Therapy
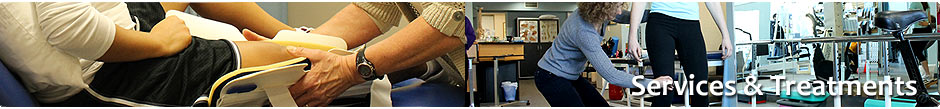
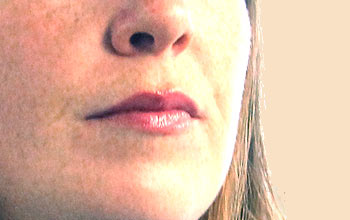 Facial Neuropathy is a condition in which the 7th cranial nerve (from the brain) becomes damaged. This damage causes facial paralysis on one side of the face. The most common causes of facial neuropathy are Bell’s Palsy (temporary facial paralysis most commonly felt to be related to a viral or bacterial infection), Acoustic Tumor (a benign tumor growing from the balance and hearing nerves), or a congenital condition (one you are born with). There are other causes of facial neuropathy, however they are less common.
Facial Neuropathy is a condition in which the 7th cranial nerve (from the brain) becomes damaged. This damage causes facial paralysis on one side of the face. The most common causes of facial neuropathy are Bell’s Palsy (temporary facial paralysis most commonly felt to be related to a viral or bacterial infection), Acoustic Tumor (a benign tumor growing from the balance and hearing nerves), or a congenital condition (one you are born with). There are other causes of facial neuropathy, however they are less common.
Signs and Symptoms of Facial Paralysis:
- Inability to close the eye on the affected side
- Drooping of the affected side (suddenly or slowly over 24 hours)
- Teariness or dryness of the eye
- Pain in or behind your ear
- Sensitivity to sound
- Drooling
- Loss of sense of taste
At the first sign of facial paralysis you must seek medical care. During the early days it is important to protect the eye. If you do not protect the eye adequately you can cause permanent damage to the cornea. A facial therapist is able to give you strategies to protect your eye.
At the early stages the facial therapist is able to take your history and assess the ability to move all the muscles of the face. If you have some ability to move the muscles of the face you will be given a treatment plan and home exercise program to assist in the recovery of the muscles. Our goal is to teach you how to use the weak side of your face and also to teach you to use both sides of your face together.
Recovery can have some challenges. Using the facial muscles has always been very automatic. You will have to learn new strategies to promote more normal movements of facial expressions. Your facial therapist will assist with these strategies. These movement control exercises will help to improve the coordination of your facial muscles, refine your facial movement for specific function (for example closing the eye), refine the movements for facial expressions such as smiling and correct the abnormal patterns of facial movement (synkinesis).
Your facial therapist is trying to coach you to use your face as normally as possible through the different stages of your recovery.
TMJ DYSFUNCTION
TMJ dysfunction is an umbrella term covering acute or chronic pain in the temporomandibular joints (or the jaw joints). The temporomandibular joint is subject to problems similar to those that affect other joints in the body such as arthritis, trauma, dislocations, and subluxations. The most common symptom of TMJ dysfunction is pain, which can be located at the jaw joint in front of the ear, or along the side of the face, or it can come in the form of headaches. TMJ problems can also lead to reduced function of the jaw, interfering with such things as eating, yawning, talking, laughing and smiling. Other common symptoms of TMJ dysfunction are clicking, popping, decreased ability to open the mouth, jaws that lock open or closed, and decreased ability to chew.
The exact cause of your pain can sometimes be difficult to determine. Most TMJ disorders can be managed with conservative care. A physiotherapist will assess your TMJ dysfunction by taking a thorough history. Questions will determine if you have any habits that are contributing to pain in the TMJ area. An assessment will be done analyzing the amount of movement, the quality of movement, the muscle tone and abnormal movement patterns during opening of the mouth. Some of the factors that cause strain and contribute to pain in the TMJ are bruxism (grinding or clenching the teeth), trauma, frequent or prolonged dental work, mal-alignment of the surfaces of the teeth, habits such as excessive gum chewing, nail biting, eating very hard foods, and poor posture.
There are a variety of treatment approaches. Your physiotherapist will work closely with your dentist to optimize your joint position and decrease the stress on the joint. In addition, we will use strategies to decrease pain and improve the muscle coordination around the joint. We will advise you of a home exercise program and outline a treatment plan.
Most people with TMJ dysfunction improve with treatment and can use the strategies at home to self-treat and control symptoms. Your physiotherapist will guide you through this process.