Lymphedema Therapy
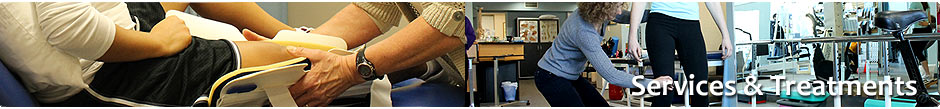
What is Lymphedema?
For starters, your lymphatic system is made up of lymph vessels that connect to lymph nodes which are found in your armpits, neck and groin. The role of your lymphatic system is significant, it supports immune function and circulation. Lymph vessels are tasked with moving fluid out of tissues and in the process waste products, dead cells, sizeable molecules of protein and dead cells get collected. The waste products are delivered to the lymph nodes to be broken down and then eliminated, while the protein-rich fluid is returned to the heart for recirculation. However, if the lymph vessels aren’t able to return the lymph fluid back into circulation it begins to accumulate which results in chronic swelling. Lymphedema is the build-up of this protein-rich lymph fluid. And swelling will likely continue to increase without the introduction of a meaningful treatment program.
You may be at risk of developing lymphedema if you’ve undergone any of the following procedures:
- Mastectomies
- Lumpectomies
- Radiation treatment
- Lymph node removal
- Surgeries, infections, or trauma to the limbs
Alternately if at birth, during childhood years or as a young adult you were diagnosed with lymphedema the information that follows will help you grasp what lymphedema is and the ways in which it can be managed.
There are two types of Lymphedema: Primary and Secondary
Primary Lymphedema is a result of abnormalities within the lymphatic system and are most common in women. Symptoms may exist from birth or can develop later on during puberty or pregnancy. Primary lymphedema is most common in the legs but can also appear in the arms or torso. Lymphedema usually occurs in one leg or arm but can surface in both arms or legs. It can also surface in hands, feet, chest, back, abdomen, face and genitals.
Secondary Lymphedema arises due to damage to the lymphatic system. Some of the most common causes are connected to surgical procedures like mastectomies and lumpectomies with radiation and/or the removal of lymph nodes. The occurrence of secondary lymphedema is usually in the arms but can also develop in the legs. Traumatic injury, infection or serious chronic venous insufficiency are additional causes.
What are the Signs or Symptoms?
The most obvious sign of lymphedema is swelling along with “pitting”. Pitting is when an area of skin is pushed in for a few seconds and the resulting indentation doesn’t disappear right away. Other signs include tightness or heaviness in the affected area or skin texture changes. You might even notice articles of clothing or jewelry fitting tighter.
And when symptoms surface external assistance and support are needed. Once the lymphatic system is compromised, the body has to work much harder to aid in the circulation of fluid. Once it’s unable to keep up with the demand the buildup of fluid results. Treatment should start at the onset otherwise it can become chronic.
How is Lymphedema treated?
At the completion of a proper diagnosis, the typical treatment procedures would be presented and discussed. There is no cure for lymphedema, the objectives become the reduction of swelling and maintaining the achieved curtailment. Most patients can experience these outcomes under a specially trained therapist conducting a skillful application of CDT (or Complete Decongestive Therapy) which is safe, reliable and non-invasive. There’s a proven track record of positive long-term outcomes for both primary and secondary lymphedema.
The CDT treatment consists of 4 components:
- Manual Lymph Drainage
- Graduated Compression Garments or Bandages
- Meticulous Skin Care
- Therapeutic Exercises
The treatment process consists of two phases. The first phase consists of reducing the swelling in the affected area by moving out the lymph fluid using Manual Lymph Drainage (MLD) techniques and bandaging. These treatments work best when performed daily for 2 – 4 weeks based on the severity of the condition. Once a reduction in swelling is achieved, the second phase begins which consists of a fitting for a graduated compression garment. The patient will play a large role during this phase through their ongoing self-care which includes wearing compression garments, maintaining meticulous skincare and performing self-manual drainage. Therapeutic exercises will also work towards supporting continued success.
York Rehab has a Certified Lymphedema Therapist fully versed in Complete Decongestive Treatment. If you have Lymphedema or suspect the onset, contact us right away.